Legal & Ethical Nursing Practice – SNB EXAM PREPARATION
🩺 Informed Consent – Exam Description
Definition:
Informed consent is a legal and ethical process in which a patient is given complete information about their condition, treatment, risks, benefits, and alternatives, and then voluntarily agrees to the procedure.

🔑 Key Elements (VERY IMPORTANT for exams)
- Disclosure – Patient receives full information
- Understanding – Patient understands what is explained
- Voluntariness – Decision is made without pressure
- Competence – Patient is mentally capable
- Consent – Agreement is given (verbal/written)
📌 Types of Consent
- Implied consent – Through actions (e.g., extending arm for injection)
- Expressed consent – Verbal or written agreement
- Informed consent – Full knowledge + voluntary decision
👩⚕️ Nurse’s Responsibilities
- Explain procedure in simple language
- Ensure patient understands
- Witness consent form (in some settings)
- Respect patient’s right to refuse
- Document properly
⚖️ Legal Importance
- Protects patient autonomy
- Protects nurse from legal issues
- Required before surgeries & major procedures
❗ Common Exam Points / Traps
- Consent is invalid if:
- Patient is unconscious (except emergency)
- Given under pressure
- Patient doesn’t understand
- Signature alone ≠ valid consent
🧠 One-line Revision (for last minute)
👉 “Informed consent = full information + understanding + voluntary agreement by a competent patient.”
SNB EXAM PRACTICE TEST BOOK PDF VOL 1 & 2 COMBINED
🔐 Confidentiality & Privacy – Exam Description
Definition:
Confidentiality is the legal and ethical duty of a nurse to keep patient information private and disclose it only to authorized persons.
Privacy refers to the patient’s right to personal space and control over their information.
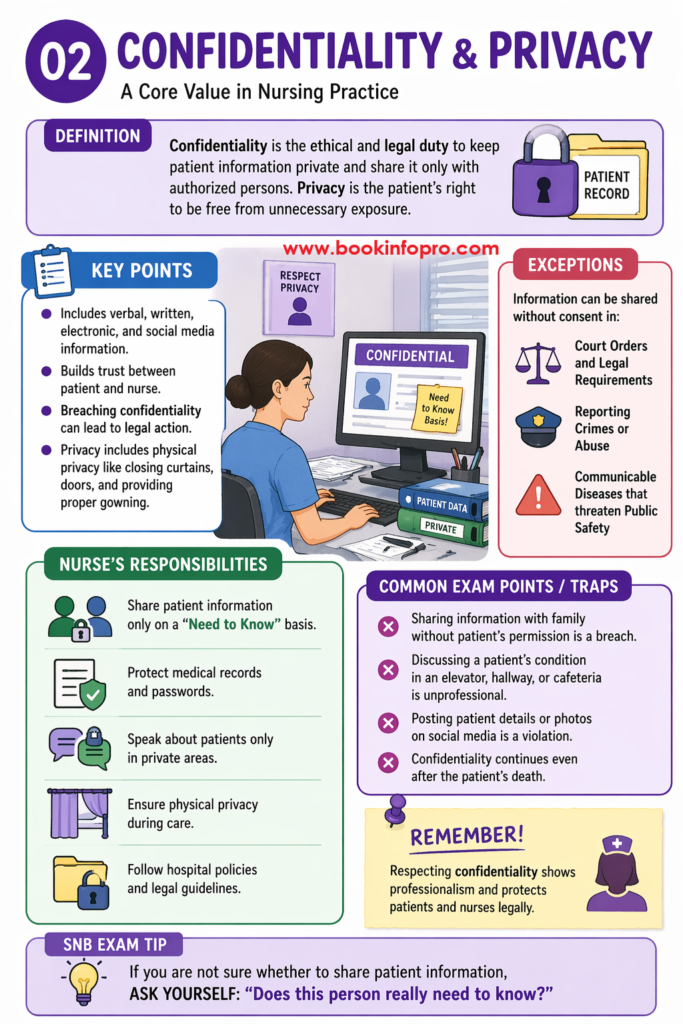
🔑 Key Points (Important for SNB)
- Includes verbal, written, electronic, and social media information
- Builds trust between patient and nurse
- Breach can lead to legal action & loss of license
- Privacy also includes:
- Physical privacy (curtains, doors)
- Respect during procedures
👩⚕️ Nurse’s Responsibilities
- Share information only on a “Need to Know” basis
- Protect medical records & passwords
- Discuss patients only in private areas
- Maintain dignity during care
- Follow hospital policies & legal guidelines
⚖️ Exceptions (VERY IMPORTANT)
Confidentiality can be broken without consent in:
- Court orders / legal requirements
- Reporting abuse or crimes
- Communicable diseases (public safety)
❗ Common Exam Traps
- Sharing info with relatives without consent ❌
- Talking about patients in public places ❌
- Posting patient details on social media ❌
- Confidentiality continues even after death ✔️
🧠 One-line Revision
👉 “Confidentiality = protect patient information; share only when legally or professionally required.”
⚖️ Negligence & Malpractice – Exam Description
Definition:
- Negligence: Failure to provide care that a reasonably competent nurse would provide, resulting in harm to the patient.
- Malpractice: A type of negligence by a professional nurse that leads to injury or damage and has legal consequences.
🔑 4 Elements of Negligence (VERY IMPORTANT – frequently asked)
- Duty of Care – Nurse has responsibility to care for the patient
- Breach of Duty – Failure to meet standard care
- Damage (Injury) – Patient is harmed
- Causation – Direct link between breach and injury
👉 All 4 must be present to prove negligence

📌 Common Causes
- Medication errors
- Failure to monitor patient
- Poor communication
- Ignoring patient complaints
- Not following standard precautions
- Incomplete documentation
👩⚕️ Nurse’s Responsibilities (Prevention)
- Follow standards & protocols
- Proper assessment, planning, implementation, evaluation
- Double-check medications
- Maintain accurate documentation
- Communicate clearly with healthcare team
❗ Common Exam Traps
- Not all mistakes = negligence ❌
- Good intention ≠ legal protection ❌
- Poor documentation can be considered negligence ✔️
⚠️ Example (Important)
👉 Giving wrong medication dose leading to harm = negligence → may become malpractice case
🧠 One-line Revision
👉 “Negligence = failure to meet standard care causing harm; malpractice = professional negligence with legal liability.”
⚖️ Nursing Ethics Principles – Exam Description
Definition:
Nursing ethics are moral principles that guide nurses in providing care that is safe, respectful, legal, and patient-centered.
🔑 Key Principles (VERY IMPORTANT – must memorize)
- Autonomy
- Respect patient’s right to make their own decisions
- Example: Allowing a patient to refuse treatment
- Beneficence
- Do what is best for the patient
- Promote health and well-being
- Non-maleficence
- “Do no harm”
- Avoid causing injury or suffering
- Justice
- Treat all patients fairly and equally
- No discrimination
- Fidelity
- Keep promises and maintain trust
- Be loyal and truthful
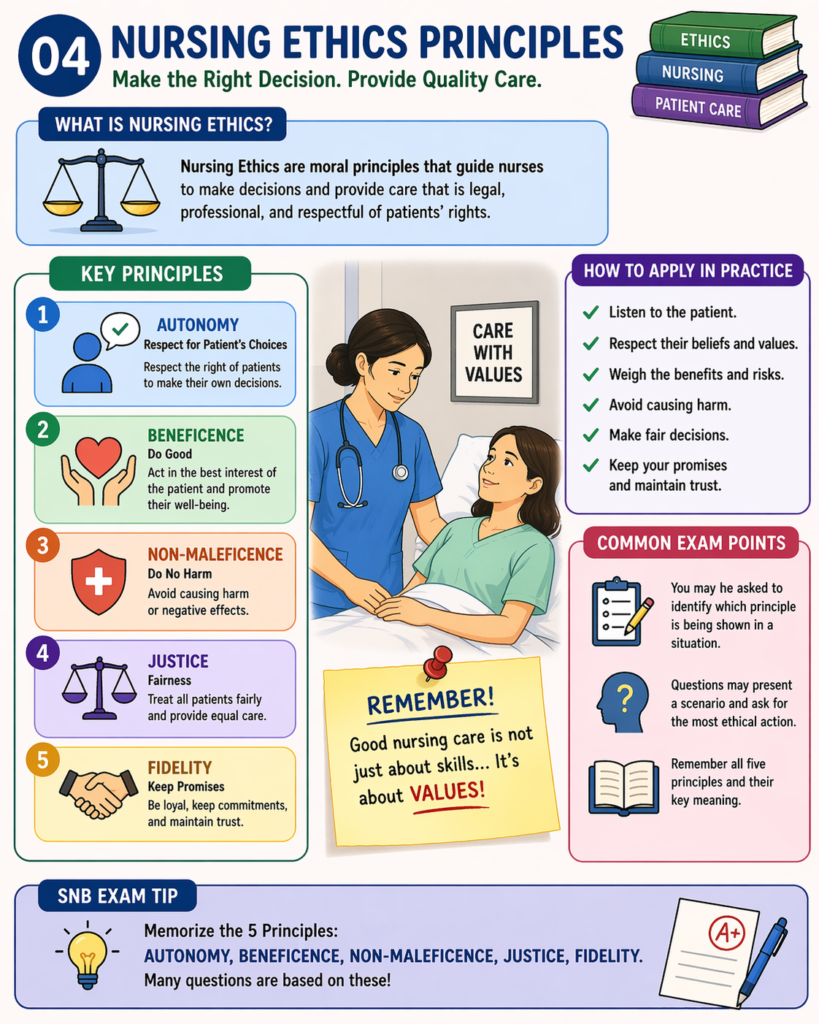
👩⚕️ Application in Practice
- Listen to patient concerns
- Respect beliefs and values
- Balance risks and benefits
- Provide safe and fair care
- Maintain trust and honesty
❗ Common Exam Points
- Identify which principle is used in a scenario
- Questions often test ethical decision-making
- All 5 principles must be clearly understood
⚠️ Example-Based Understanding
- Patient refuses surgery → Autonomy
- Giving pain relief → Beneficence
- Avoiding wrong medication → Non-maleficence
- Equal treatment → Justice
- Keeping patient information confidential → Fidelity
🧠 One-line Revision
👉 “Ethics = doing the right thing using 5 principles: autonomy, beneficence, non-maleficence, justice, fidelity.”
⚖️ Legal Safeguards in Nursing Practice – Exam Description
Definition:
Legal safeguards are laws, rules, and professional actions that protect both patients’ rights and nurses from legal liability while delivering care.
🔑 Key Legal Safeguards (VERY IMPORTANT)
- Practice within Scope
- Perform only those duties you are trained and authorized to do
- Avoid performing procedures beyond your competency
- Follow Laws & Policies
- Adhere to hospital policies, nursing standards, and legal guidelines
- Follow physician’s orders correctly
- Obtain Informed Consent
- Ensure patient understands and agrees before procedures
- Essential for surgeries and invasive treatments
- Maintain Confidentiality
- Protect patient information
- Share only on a need-to-know basis
- Accurate Documentation
- Record care clearly, promptly, and completely
- “If it’s not documented, it’s not done” (important exam concept)
- Follow Standard Precautions
- Infection control measures
- Ensure patient and nurse safety

👩⚕️ Importance
- Prevents lawsuits and legal action
- Ensures safe and quality care
- Builds trust with patients
- Supports professional accountability
❗ Common Exam Points
- Questions on documentation importance
- Identifying legal vs illegal nursing actions
- Role of consent and confidentiality
- Choosing correct action in clinical scenarios
⚠️ Key Reminder
👉 Good documentation = Best legal protection
🧠 One-line Revision
👉 “Legal safeguards = follow law, stay within scope, document properly, protect patient rights.”
👩⚕️ Professional Conduct & Code of Ethics – Exam Description
Definition:
- Professional Conduct: The way a nurse behaves, communicates, and performs duties in a professional setting.
- Code of Ethics: A set of guiding principles that ensure nursing care is safe, respectful, and ethical.
🔑 Key Principles of Professional Conduct (IMPORTANT)
- Respect
- Treat patients, families, and colleagues with dignity
- Integrity
- Be honest and do the right thing even when not observed
- Competence
- Work within your knowledge and skills
- Continue learning
- Accountability
- Take responsibility for your actions and decisions
- Confidentiality
- Protect patient information at all times
- Professionalism
- Be punctual, reliable, and maintain proper behavior

👩⚕️ Nurse’s Responsibilities
- Follow Code of Ethics and standards
- Provide safe and quality care
- Respect patient rights, culture, and values
- Communicate professionally
- Maintain trust and integrity
❗ Common Exam Points
- Define professional conduct vs code of ethics
- Identify unprofessional behavior (e.g., rude communication, negligence)
- Questions on accountability and integrity
- Choosing correct ethical action in scenarios
⚠️ Key Reminder
👉 Your behavior reflects the entire nursing profession
🧠 One-line Revision
👉 “Professional conduct = respectful, responsible behavior; code of ethics = principles guiding that behavior.”
🧠 Ethical Decision Making – Exam Description
Definition:
Ethical decision making is the process nurses use to make right, fair, and patient-centered decisions when faced with difficult situations.
🔑 Steps of Ethical Decision Making (VERY IMPORTANT)
- Identify the Problem
- What is the ethical issue?
- Gather Information
- Patient condition, facts, values, beliefs
- Identify Options
- List all possible actions
- Apply Ethical Principles
- Autonomy, Beneficence, Non-maleficence, Justice, Fidelity
- Choose the Best Action
- Select safest and most ethical option
- Implement the Decision
- Act and provide care
- Evaluate the Outcome
- Was it effective? Any improvements needed?

⚖️ Principles Involved
- Autonomy – Respect patient choice
- Beneficence – Do good
- Non-maleficence – Avoid harm
- Justice – Be fair
- Fidelity – Keep trust
⚠️ Example (IMPORTANT)
👉 Patient refuses treatment due to beliefs
✔ Respect decision (Autonomy)
✔ Provide information
✔ Support patient rights
👩⚕️ Key Points for Practice
- Always put patient first
- Consider risks vs benefits
- Communicate with healthcare team
- Document decisions properly
❗ Common Exam Points
- Arrange steps in correct order
- Identify ethical principle in scenario
- Choose best action in difficult situation
🧠 One-line Revision
👉 “Ethical decision making = identify problem → apply principles → choose best patient-centered action.”
💊 5 Rights of Medication Administration – Exam Description
Definition:
The 5 Rights are essential safety principles nurses follow to ensure correct and safe medication administration.
🔑 The 5 Rights (VERY IMPORTANT – MUST MEMORIZE)
- Right Patient
- Confirm identity using ID band / name / DOB
- Right Drug
- Check medication label 3 times
- Right Dose
- Give correct dose as prescribed
- Double-check calculations
- Right Route
- Ensure correct method (oral, IV, IM, SC, etc.)
- Right Time
- Administer at correct time and frequency

👩⚕️ Steps to Administer Safely
- Check doctor’s order
- Verify patient identity
- Compare with MAR (Medication Administration Record)
- Check drug label carefully
- Assess patient condition
- Administer medication
- Document and monitor response
⚠️ Example (Important)
👉 Giving medication to wrong patient = medication error → can cause serious harm
❗ Common Exam Points
- List all 5 Rights
- Identify which right is violated in a scenario
- Importance of checking ID and label
- Steps of safe medication administration
💡 Key Tips
- Never rely on memory
- Always double-check
- When in doubt → ask
⚠️ Key Reminder
👉 “5 Rights followed = Patient Safety ensured”
🧠 One-line Revision
👉 “Right patient + drug + dose + route + time = safe medication administration.”
🦠 Infection Control & Patient Safety – Exam Description
Definition:
Infection control refers to the measures taken to prevent the spread of infections, while patient safety ensures protection from harm during healthcare.
🔑 Importance (VERY IMPORTANT)
- Prevents spread of infections
- Protects patients, nurses, and visitors
- Reduces hospital-acquired infections (HAIs)
- Improves patient outcomes
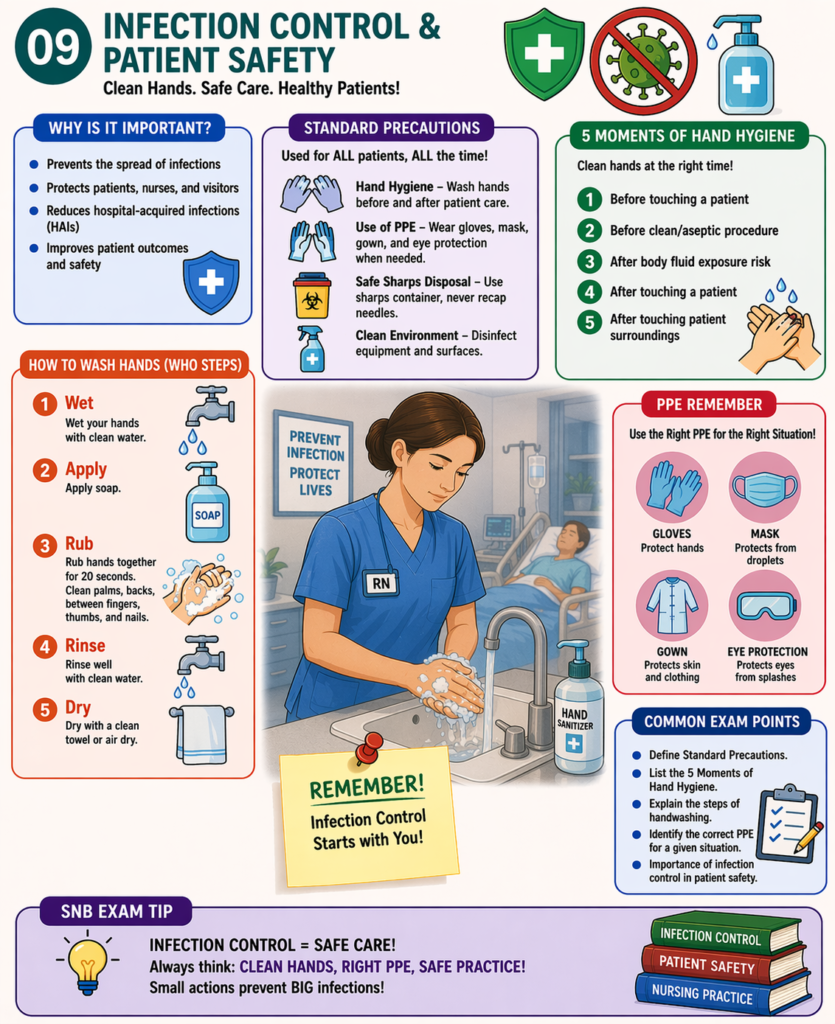
🛡️ Standard Precautions (MUST KNOW)
- Apply to all patients, all the time
- Hand hygiene before & after care
- Use PPE (gloves, mask, gown, eye protection)
- Safe disposal of sharps
- Clean and disinfect equipment & environment
✋ 5 Moments of Hand Hygiene (VERY IMPORTANT)
- Before touching patient
- Before clean/aseptic procedure
- After body fluid exposure
- After touching patient
- After touching patient surroundings
🧼 Steps of Handwashing (WHO)
- Wet hands
- Apply soap
- Rub for 20 seconds
- Rinse
- Dry
🧤 PPE Use
- Gloves – protect hands
- Mask – prevent droplet spread
- Gown – protect clothing/skin
- Eye protection – prevent splashes
❗ Common Exam Points
- Define standard precautions
- List 5 moments of hand hygiene
- Steps of handwashing
- Identify correct PPE use in scenarios
⚠️ Key Reminder
👉 Infection control starts with YOU (the nurse)
🧠 One-line Revision
👉 “Clean hands + proper PPE + standard precautions = patient safety.”
💬 Nursing Communication & Therapeutic Relationship – Exam Description
Definition:
- Nursing Communication: Process of sharing information, feelings, and ideas between nurse and patient.
- Therapeutic Relationship: A professional, trust-based relationship that promotes healing and quality care.
🔑 Principles of Therapeutic Communication (VERY IMPORTANT)
- Active Listening
→ Give full attention, don’t interrupt - Clear Communication
→ Use simple, respectful language - Empathy
→ Understand patient’s feelings - Confidentiality
→ Protect patient information - Respect
→ Value patient’s beliefs and choices
👩⚕️ Steps to Build Therapeutic Relationship
- Introduce yourself
- Use patient’s name
- Explain procedures clearly
- Listen and respond appropriately
- Build trust (honesty + confidentiality)

🌟 Qualities of a Good Nurse
- Kind and compassionate
- Good listener
- Patient and calm
- Respectful
- Trustworthy
- Non-judgmental
- Professional
💡 Benefits
- Builds trust and cooperation
- Improves patient satisfaction
- Promotes healing
- Reduces anxiety
- Helps in accurate assessment
❗ Common Exam Points
- Define therapeutic communication
- Identify effective vs ineffective communication
- Choose best nurse response in scenarios
- Importance of empathy and listening
⚠️ Key Reminder
👉 Listening is more important than talking
🧠 One-line Revision
👉 “Therapeutic communication = listen, understand, respect, and build trust.”
